
GETTING THE CLAIMS ACCEPTED, ON THE FIRST SUBMISSION!
Insurance eligibility verification is the most important and the first step in the medical billing process. Research confirms that most of the claims are denied or delayed due to inadequate or incorrect coverage information provided by the patients during visits and current coverage information not updated by the office / hospital staff. This lack of or improper insurance eligibility verification directly impacts the reimbursements.
Why opt for insurance eligibility verification
Insurance companies regularly make policy changes and updates in their health plans. Therefore, it is important for the medical billing company or the provider to verify if the patient is covered under the new plan to get maximum reimbursement. Confirming the insurance coverage facilitates acceptance of the claim on the first submission, whereas non-verification leads to several discomforts like rework, decreased patient satisfaction and increased errors other than causing delays and denials.
At MD CAVE, we understand the importance of insurance eligibility verification.
Help in Increasing Revenue
Minimize delays and denials considerably
Improve collections by reducing write-offs

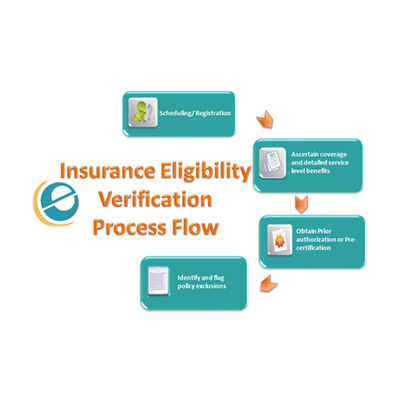
Insurance eligibility verification process at e-care :
Receive Schedules of patients via EDI, email or fax or check them every day in the appointment scheduling software.
Verify patients’ insurance coverage with primary and secondary payers by making calls to the payers and checking through their authorized online insurance portals. We also contact patients for additional information, if required
Update the medical billing system with eligibility and verification details such as member ID, group ID, coverage period, co-pay, Deductible and co-insurance information and other code level benefits information including max limits allowed.
In case of issues regarding a patient’s eligibility, we inform the client immediately
MD CAVE dedicated insurance eligibility verification team delivers a thorough verification, thereby aiding dramatic reduction of the clients’ accounts receivable cycle.

